

The viral therapy was tested in three elderly animals with spontaneous brain tumors by a group affiliated with the FAPESP-funded Human Genome and Stem Cell Research Center (immunofluorescence image of brain tumor tissue from a dachshund dog after intrathecal injections of Zika virus. The presence of the virus [red] infecting tumor cells [blue] with intense necrosis is observed at the edges of the tumor. These results reinforce the tropism of Zika virus and its potential as oncolytic therapy a
The viral therapy was tested in three elderly animals with spontaneous brain tumors by a group affiliated with the FAPESP-funded Human Genome and Stem Cell Research Center.
The viral therapy was tested in three elderly animals with spontaneous brain tumors by a group affiliated with the FAPESP-funded Human Genome and Stem Cell Research Center.
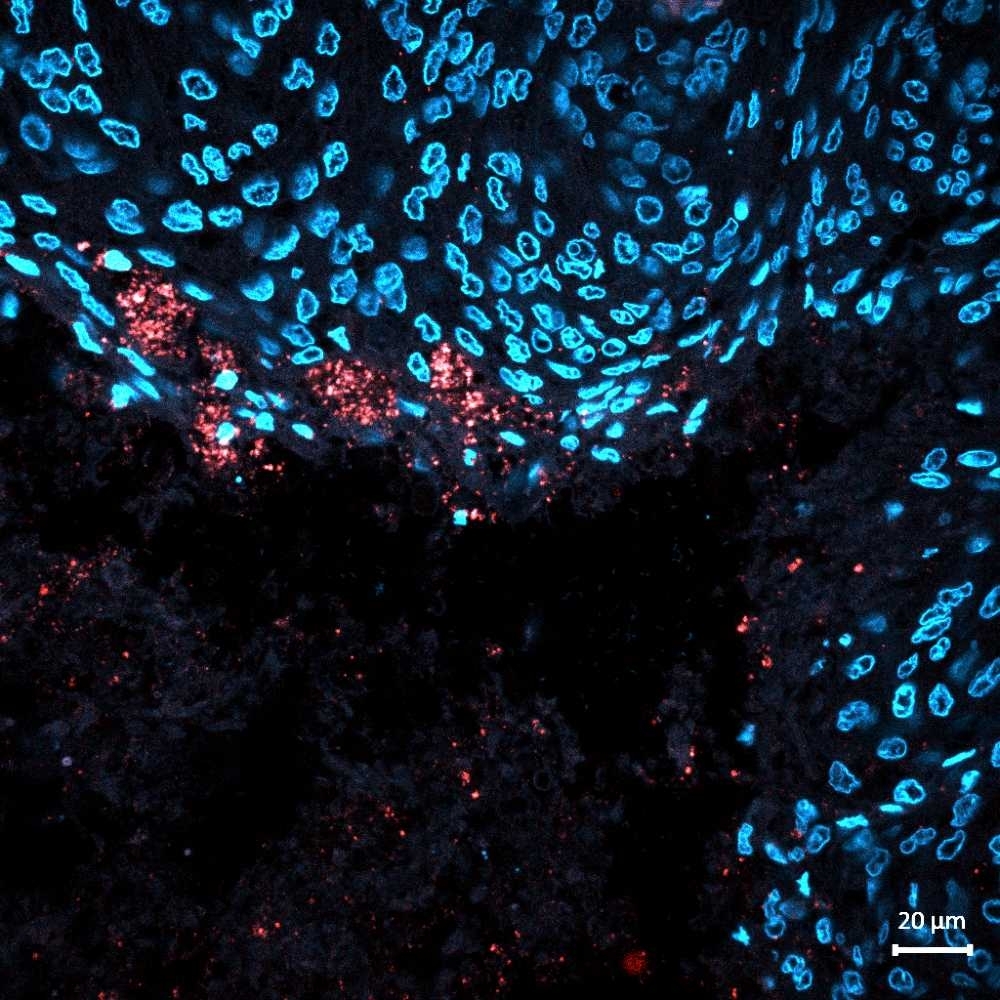
The viral therapy was tested in three elderly animals with spontaneous brain tumors by a group affiliated with the FAPESP-funded Human Genome and Stem Cell Research Center (immunofluorescence image of brain tumor tissue from a dachshund dog after intrathecal injections of Zika virus. The presence of the virus [red] infecting tumor cells [blue] with intense necrosis is observed at the edges of the tumor. These results reinforce the tropism of Zika virus and its potential as oncolytic therapy a
By Karina Toledo | Agência FAPESP – Brazilian researchers have just reported proving the potential of zika virus to combat advanced-stage central nervous system tumors in dogs. The study was published on Tuesday, March 10, in the journal Molecular Therapy.
Three elderly dogs with spontaneous brain tumors were treated with injections of zika virus by scientists affiliated with the Human Genome and Stem Cell Research Center (HUG-CELL), a Research, Innovation and Dissemination Center (RIDC) supported by FAPESP and hosted by the University of São Paulo (USP).
“We observed a surprising reversal of the clinical symptoms of the disease, as well as tumor reduction and longer survival with quality, which matters most. Moreover, the treatment was well tolerated and there were no adverse side-effects. We’re genuinely excited by the results,” Mayana Zatz, a professor at USP’s Institute of Biosciences (IB) and HUG-CELL’s principal investigator told Agência FAPESP.
The group had already demonstrated zika’s capacity to infect and destroy central nervous system tumor cells in mice (read more at: agencia.fapesp.br/27677). In this model, the formation of human tumors is induced in the laboratory, a procedure that can be performed only using immunosuppressed animals. One of the key advantages of the new study, according to the authors, was the possibility of evaluating the effects of the therapy in animals with an active immune system.
“The findings confirm that the therapy acts via two mechanisms. On one hand, the virus infects tumor cells, starts to replicate in them, and eventually kills them. On the other, it alerts the immune system to the presence of the tumor. The infection triggers an inflammatory reaction, and defense cells migrate to the site,” said Carolini Kaid, who has a postdoctoral scholarship from FAPESP and is first author of the article.
According to Kaid, central nervous system tumors respond poorly to immunotherapy because the blood-brain barrier that protects the brain from potentially toxic substances present in the blood hinders migration of defense cells to the site.
However, post-mortem analysis of the dogs’ brain tissue showed that T lymphocytes, macrophages and monocytes had infiltrated the tumor mass.
“The analysis also showed that zika was present only at the edges of the tumor. No other brain cells were affected. This is a most important finding, enhancing our confidence that the treatment is safe,” Kaid said.
Treatment protocol
Three dogs were treated by the HUG-CELL team, all of them patients of Raquel Azevedo dos Santos Madi, a veterinary physician at a private hospital in Granja Vianna, a district of metropolitan São Paulo. All three were diagnosed by MRI scans with advanced-stage cancer, when the clinical signs of the disease are evident. Without treatment, such patients survive for 20-30 days on average.
The virus was inserted into the dogs’ cerebrospinal fluid by means of an injection in the region of the spine just below the base of the skull. The virus derived from a strain isolated from a Brazilian patient (ZIKVBR). It was purified and gifted to the group by partners at the São Paulo-based Butantan Institute.
The treatment was conducted at the hospital. The animals were allowed to go home only after three negative tests for the presence of the virus in their blood and urine. “We followed a very strict protocol to avoid contaminating anyone,” Zatz said.
The first dog to receive the therapy was Pirata, a 13-year-old pit bull weighing 26 kilograms (kg). “He came to us in a pre-coma. He was unable to stand up and his only source of nutrients was an IV drip. Three days after the injection, he was able to eat again, stand up and even take a few steps. He survived for 14 days but was already very weak and suffered a cardiac arrest. His owners had to put him down,” Zatz said.
The longest survival time was observed in Matheus, an eight-year-old boxer weighing 32 kg. This dog survived for 150 days after the therapy. An MRI scan showed 35.5% tumor reduction.
The third patient treated was Nina, a 12-year-old dachshund weighing 6.4 kg. This animal survived for 80 days, with 37.92% tumor reduction.
“In contrast with the effects of chemotherapy, the animals displayed no negative reactions to the treatment. We began with a small dose, which was well tolerated, so we injected a second dose that was ten times larger,” Zatz said.
Versatile therapy
The type of tumor was confirmed in each dog by post-mortem histopathology. The boxer had an oligodendroglioma, and the dachshund an intracranial meningioma. “We were unable to identify the pit bull’s tumor as we found no tumor cells. The tumor was small and seems to have been eliminated,” Kaid said.
In the group’s prior experiments with mice, zika destroyed tumor cell lines derived from medulloblastoma and atypical teratoid/rhabdoid tumor (AT/TR), central nervous system cancers of embryonic origin that usually manifest in children. The researchers also conducted in vitro tests in which they observed zika’s potential to infect and destroy glioblastoma and ependymoma cells.
According to Oswaldo Keith Okamoto, a professor at IB-USP and a member of HUG-CELL, the data suggests viral therapy may be applicable to several types of central nervous system cancer in both children and patients over the age of 60. “These two groups tend to suffer more often than not from aggressive types of tumor, for which there are no effective treatments at present,” he said.
For over fifteen years, Okamoto has investigated strategies for destroying tumor cells with similar characteristics to stem cells. Although they cannot differentiate into any other type of cell, these “tumor stem cells” make the disease more aggressive and hard to treat (read more at: agencia.fapesp.br/21959/).
The in vitro studies performed by the HUG-CELL group compared the virus’s interactions with “tumor stem cells” and healthy neural progenitor cells, a type of brain stem cell that gives rise to neurons, astrocytes and oligodendrocytes, among other nerve cells.
“When we infect the neural progenitor cells, zika interrupts their proliferation, and some of them die. But the spheres [formed when progenitor cells cluster together in 3D culture] remain relatively intact. In the case of tumor stem cells, the destruction is far more prominent. Our in vitro tests also showed that the virus doesn’t infect mature nerve cells such as neurons. That’s a very positive finding,” Kaid said.
According to Okamoto, groups in the United Kingdom and Greece are interested in leading collaborative projects in search of a better understanding of zika’s action mechanism in tumor stem cells.
In parallel, the HUG-CELL researchers are refurbishing the dog kennels at IB-USP in preparation for the installation of an intensive care unit for use in further studies. “We learned a great deal from the study with these three dogs, and we now plan to begin a new preclinical trial with a larger number of animals. One of our aims is to discover the ideal dose of the virus for the treatment. If it works, it will offer hope that both dogs and humans can be given the treatment, but we’ll need more funding and we’re looking for partners,” Zatz said.
The article “Safety, tumor reduction and clinical impact of Zika virus injection in dogs with advanced-stage brain tumors” can be read at www.cell.com/action/showPdf?pii=S1525-0016%2820%2930138-6.
Republish
The Agency FAPESP licenses news via Creative Commons (CC-BY-NC-ND) so that they can be republished free of charge and in a simple way by other digital or printed vehicles. Agência FAPESP must be credited as the source of the content being republished and the name of the reporter (if any) must be attributed. Using the HMTL button below allows compliance with these rules, detailed in Digital Republishing Policy FAPESP.





