


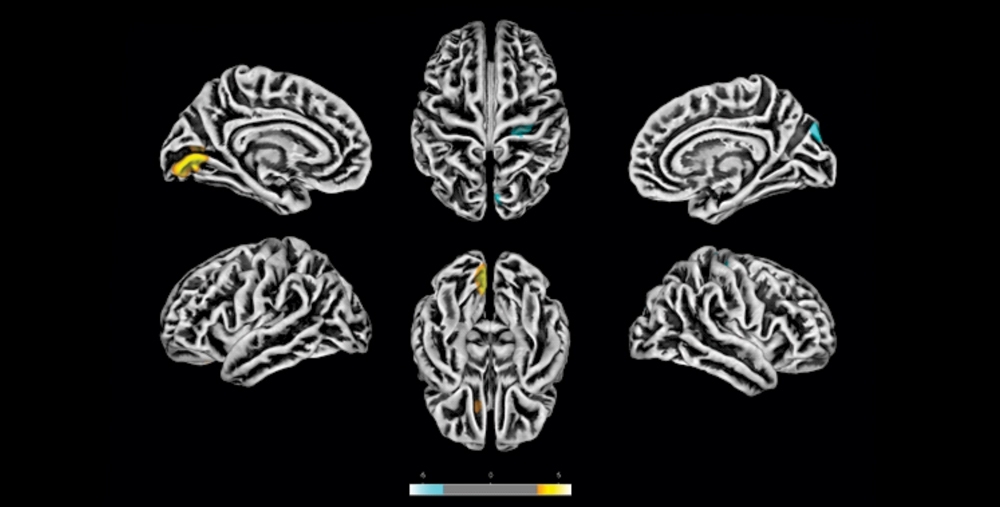
MRI scans performed at the University of Campinas on 81 patients with post-COVID neuropsychiatric symptoms reveal alterations to structure of cerebral cortex. Cortical thickness is decreased in some areas (shaded yellow) and increased in others (blue) (image: www.medrxiv.org/content/10.1101/2020.10.09.20207464v1)
Led by research groups from the universities of Campinas and São Paulo, the investigation combined MRI scans of mild COVID-19 patients, analysis of brain tissue samples from patients who died from COVID-19, and experiments performed with human nerve cells infected in the laboratory.
Led by research groups from the universities of Campinas and São Paulo, the investigation combined MRI scans of mild COVID-19 patients, analysis of brain tissue samples from patients who died from COVID-19, and experiments performed with human nerve cells infected in the laboratory.
MRI scans performed at the University of Campinas on 81 patients with post-COVID neuropsychiatric symptoms reveal alterations to structure of cerebral cortex. Cortical thickness is decreased in some areas (shaded yellow) and increased in others (blue) (image: www.medrxiv.org/content/10.1101/2020.10.09.20207464v1)
By Karina Toledo | Agência FAPESP - A Brazilian study reported on October 13 on the medRxiv platform proves that SARS-CoV-2 can infect brain tissue cells, particularly astrocytes. The findings also show that the virus may cause significant alterations in the structure of the cortex even in mild COVID-19 patients.
The cerebral cortex is the outer layer of gray matter over the hemispheres. It is the largest site of neural integration in the central nervous system and plays a key role in complex functions such as memory, attention, consciousness, and language.
The investigation was conducted by several groups at the University of Campinas (UNICAMP) and the University of São Paulo (USP), all funded by FAPESP. Researchers at the Brazilian Biosciences National Laboratory (LNBio), D'Or Institute (IDOR) and the Federal University of Rio de Janeiro (UFRJ) also contributed to the study.
“Two previous studies detected the presence of the novel coronavirus in the brain, but no one knew for sure if it was in the bloodstream, endothelial cells [lining the blood vessels] or nerve cells. We showed for the first time that it does indeed infect and replicate in astrocytes, and that this can reduce neuron viability,” Daniel Martins-de-Souza, one of the leaders of the study, told Agência FAPESP. Martins-de-Souza is a professor at UNICAMP’s Biology Institute and a researcher affiliated with IDOR.
Astrocytes are the most abundant central nervous system cells. Their functions include providing biochemical support and nutrients for neurons; regulating levels of neurotransmitters and other substances that may interfere with neuronal functioning, such as potassium; maintaining the blood-brain barrier that protects the brain from pathogens and toxins; and helping to maintain brain homeostasis.
Infection of astrocytes was confirmed by experiments using brain tissue from 26 patients who died of COVID-19. The tissue samples were collected during autopsies conducted using minimally invasive procedures by Alexandre Fabro, a pathologist and professor at the University of São Paulo’s Ribeirão Preto Medical School (FMRP-USP). The analysis was coordinated by Thiago Cunha, also a professor in FMRP-USP and a member of the Center for Research on Inflammatory Diseases (CRID).
The researchers used a technique known as immunohistochemistry, a staining process in which antibodies act as markers of viral antigens or other components of the tissue analyzed. “For example, we can insert one antibody into the sample to turn the astrocytes red on binding to them, another to mark the SARS-CoV-2 spike protein by making it green, and a third to highlight the virus’s double-stranded RNA, which only appears during replication, by turning it magenta,” Martins-de-Souza explained. “When the images produced during the experiment were overlaid, all three colors appeared simultaneously only in astrocytes.”
According to Cunha, the presence of the virus was confirmed in the 26 samples analyzed. Alterations suggesting possible damage to the central nervous system were also found in five samples.
“In these five samples we observed signs of necrosis and inflammation, such as edema [swelling caused by a buildup of fluid], neuronal lesions and inflammatory cell infiltrates,” he said. “But we only had access to a small part of these brains, and similar signs may have been present in different regions of the brains of the other 21 patients.”
Persistent symptoms
In another part of the research, conducted in UNICAMP’s School of Medical Sciences (FCM), 81 volunteers who had recovered from mild COVID-19 were submitted to magnetic resonance imaging (MRI) scans of their brains. These scans were performed 60 days after diagnostic testing on average. A third of the participants still had neurological or neuropsychiatric symptoms at the time. They complained mostly of headache (40%), fatigue (40%), memory alterations (30%), anxiety (28%), loss of smell (28%), depression (20%), daytime drowsiness (25%), loss of taste (16%) and low libido (14%).
“We posted a link for people interested in participating in the trial to register, and were surprised to get more than 200 volunteers in only a few days. Many were polysymptomatic, with widely varying complaints. In addition to the neuroimaging exam, they’re being evaluated neurologically and taking standardized tests to measure performance in cognitive functions such as memory, attention and mental flexibility. In the article we present the initial results,” said Clarissa Yasuda, a professor and member of the Brazilian Research Institute for Neuroscience and Neurotechnology (BRAINN).
Only volunteers diagnosed with COVID-19 by RT-PCR and not hospitalized were included in the study. The assessments were carried out after the end of the acute phase, and the results were compared with data for 145 healthy uninfected subjects.
The MRI scans showed that some volunteers had decreased cortical thickness in some brain regions compared with the average for controls, and increased cortical thickness in others, possibly indicating some degree of edema, according to the authors.
“We observed atrophy in areas associated, for example with anxiety, one of the most frequent symptoms in the study group,” Yasuda said. “Considering that the prevalence of anxiety disorders in the Brazilian population is 9%, the 28% we found is an alarmingly high number. We didn’t expect these results in patients who had had the mild form of the disease.”
In neuropsychological tests designed to evaluate cognitive functioning, the volunteers also underperformed in some tasks compared with the national average. The results were adjusted for age, sex and educational attainment, as well as the degree of fatigue reported by each participant.
“The question we’re left with is this: Are these symptoms temporary or permanent?” Yasuda said. “To find out, we plan to continue monitoring these volunteers for some time.”
Energy metabolism affected
In IB-UNICAMP’s Neuroproteomics Laboratory, which is headed by Martins-de-Souza, experiments were performed on brain tissue cells from people who died of COVID-19 and astrocytes cultured in vitro to find out how infection by SARS-CoV-2 affects nervous system cells from the biochemical standpoint.
The autopsy samples were obtained via collaboration with the group led by Paulo Saldiva, a professor at the University of São Paulo’s Medical School (FM-USP). The proteome (all proteins present in the tissue) was mapped using mass spectrometry, a technique employed to identify different substances in biological samples according to their molecular mass.
“When the results were compared with those of uninfected subjects, several proteins with altered expression were found to be abundant in astrocytes, which validated the findings obtained by immunohistochemistry,” Martins-de-Souza said. “We observed alterations in various biochemical pathways in the astrocytes, especially pathways associated with energy metabolism.”
The next step was to repeat the proteomic analysis in cultured astrocytes infected in the laboratory. The astrocytes were obtained from induced pluripotent stem cells (iPSCs). The method consists of reprogramming adult cells (derived from skin or other easily accessible tissues) to assume a stage of pluripotency similar to that of embryo stem cells. This first part was conducted in the IDOR laboratory of Stevens Rehen, a professor at UFRJ. Martins-de-Souza’s team then used chemical stimuli to make the iPSCs differentiate into neural stem cells and eventually into astrocytes.
“The results were similar to those of the analysis of tissue samples obtained by autopsy in that they showed energy metabolism dysfunction,” Martins-de-Souza said. “We then performed a metabolomic analysis [focusing on the metabolites produced by the cultured astrocytes], which evidenced glucose metabolism alterations. For some reason, infected astrocytes consume more glucose than usual, and yet cellular levels of pyruvate and lactate, the main energy substrates, decreased significantly.”
Lactate is one of the products of glucose metabolism, and astrocytes export this metabolite to neurons, which use it as an energy source. The researchers’ in vitro analysis showed that lactate levels in the cell culture medium were normal but decreased inside the cells. “Astrocytes appear to strive to maintain the energy supply to neurons even if this effort weakens their own functioning,” Martins-de-Souza said.
As an outcome of this process, the functioning of the astrocytes’ mitochondria (energy-producing organelles) was indeed altered, potentially influencing cerebral levels of such neurotransmitters as glutamate, which excites neurons and is associated with memory and learning, or gamma-aminobutyric acid (GABA), which inhibits excessive firing of neurons and can promote feelings of calm and relaxation.
“In another experiment, we attempted to culture neurons in the medium where the infected astrocytes had grown previously and measured a higher-than-expected cell death rate. In other words, this culture medium ‘conditioned by infected astrocytes’ weakened neuron viability,” Martins-de-Souza said.
Although the findings described in the article, which has yet to be peer-reviewed, confirm those of several previously published studies that pointed to possible neurological and neuropsychiatric manifestations of COVID-19, the study was more extensive in scope, he added.
“One of the most intriguing unanswered questions was whether cerebral dysfunction was caused by systemic inflammation or infection by the virus directly impaired the functioning of nerve cells. Our results show that SARS-CoV-2 can indeed penetrate brain cells and affect their functioning,” he said.
For Cunha, the next question is how the virus reaches the central nervous system and what mechanism it uses to penetrate astrocytes. The answer could offer clues to possible interventions capable of blocking infection.
“We also plan to conduct experiments with mice that have been genetically modified to express human ACE-2 [the main protein used by the virus to infect cells],” he said. “The idea is to confirm in these animals whether there’s a causal link – whether infection in and of itself can induce the alterations we observed in patients’ brains.”
According to Marcelo Mori, a professor at IB-UNICAMP and a member of the Obesity and Comorbidities Research Center (OCRC), the study was only possible thanks to the collaboration of researchers with varied and complementary backgrounds and expertise. “It demonstrates that first-class competitive science is always interdisciplinary,” he said. “It’s hard to compete internationally if you stay inside your own lab, confining yourself to the techniques with which you’re familiar and the equipment to which you have access.”
The article has 74 authors. The experiments were conducted by four postdoctoral fellows: Fernanda Crunfli, Flávio P. Veras, Victor C. Carregari and Pedro H. Vendramini.
OCRC, CRID and BRAINN are Research, Innovation and Dissemination Centers (RIDCs) funded by FAPESP. The Foundation also supported the study via funding for seven other projects: 20/04746-0, 17/25588-1, 19/00098-7, 20/04919-2, 20/05601-6, 20/04860-8, and 19/11457-8.
The article “SARS-CoV-2 infects brain astrocytes of COVID-19 patients and impairs neuronal viability” can be retrieved from: www.medrxiv.org/content/10.1101/2020.10.09.20207464v1.
Republish
The Agency FAPESP licenses news via Creative Commons (CC-BY-NC-ND) so that they can be republished free of charge and in a simple way by other digital or printed vehicles. Agência FAPESP must be credited as the source of the content being republished and the name of the reporter (if any) must be attributed. Using the HMTL button below allows compliance with these rules, detailed in Digital Republishing Policy FAPESP.





