

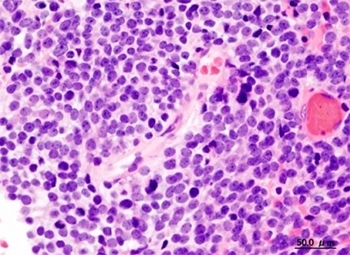
In vitro experiments were performed on cell lines derived from medulloblastoma tumors, the most common type of brain cancer in children (image: Wikimedia Commons)
The expression of genes that code for pluripotency factors is associated with shorter survival and higher risk of metastasis in medulloblastoma patients.
The expression of genes that code for pluripotency factors is associated with shorter survival and higher risk of metastasis in medulloblastoma patients.

In vitro experiments were performed on cell lines derived from medulloblastoma tumors, the most common type of brain cancer in children (image: Wikimedia Commons)
By Karina Toledo
Agência FAPESP – Researchers at the University of São Paulo’s Bioscience Institute (IB-USP) in Brazil are studying a group of human genes that, when expressed in malignant tumors, endow tumor cells with properties similar to those of stem cells, making them more aggressive and resistant to treatment.
In vitro experiments were performed with cell lines derived from medulloblastoma tumors, the most common type of brain cancer in children. Recent findings have been published in the journals Stem Cells and Development and Cancer Science.
“When these genes are expressed, they aren’t mere markers for a poor prognosis; they contribute actively to tumor aggressiveness. So they’re worth exploring as therapeutic targets,” said Oswaldo Keith Okamoto, a professor at IB-USP and a member of the Human Genome and Stem-Cell Research Center (HUG-CELL), one of the Research, Innovation and Dissemination Centers (RIDCs) supported by FAPESP.
The group led by Okamoto has focused on researching the role of four genes that code for factors relating to pluripotency: OCT4, L1TD1, LIN28 and miR-367. Instead of a protein, miR-367 codes for a microRNA, a small fragment of RNA that does not contain information for the production of proteins but plays a regulatory role in the genome.
According to Okamoto, these four genes should be predominantly expressed in embryonic stem cells that emerge in the first week after fertilization.
“At that stage the embryo consists of a structure called a blastocyst, containing a mass of embryonic stem cells that express important pluripotency factors for this stage of development,” he said.
However, expression database analysis has shown that these same genes are often expressed in medulloblastoma samples, indicating that the tumor cells are endowed with certain stem cell properties such as a high capacity for self-renewal (generating similar stem cells) and dissemination throughout the body.
Previous research by Okamoto’s group had already shown that the presence of this type of tumor stem cell correlates with shorter survival times and a higher risk of metastasis.
“Several studies have been performed in the last 15 years to understand the role of tumor stem cells, which have been observed in breast and prostate cancer as well as other types of cancer,” Okamoto said. “They’re relevant from the clinical standpoint because they’re more tumorigenic and more capable of self-renewal. They can also spread aggressively through the body and colonize remote locations. And they’re more resistant to treatment.”
According to Okamoto, it is not known exactly how tumor stem cells are produced. One hypothesis is that they are derived from the malignant transformation of normal stem cells. Another is that additional genetic alterations in already malignant cells endow them with characteristics typical of stem cells.
“For some tumors of embryonic origin, such as medulloblastoma, it’s possible that for some reason genes active in embryo stem cells aren’t switched off when they should be while the organs are maturing. If so, these cells may be unable to differentiate properly, becoming genetically unstable and giving rise to a tumor. It’s a plausible hypothesis,” he said.
Experiments
The role of the L1TD1 gene was investigated in depth during postdoctoral research by Márcia Cristina Teixeira dos Santos, supported by a scholarship from FAPESP.
Using a technique known as RNA interference, in which short RNA molecules that do not code for protein bind to the target gene’s messenger RNA and inhibit expression of the gene, the group silenced L1TD1 in two medulloblastoma cell lines to determine whether the procedure affected any properties that correlated closely with tumor aggressiveness.
Some 48 hours after silencing, without any other form of intervention, only 50% of the tumor cells remained viable. After 96 hours, approximately 80% of the cells were dead.
The capacities for cell migration and invasion, key drivers of metastasis, decreased by more than half over the 96 hours. Proliferation and resistance to apoptosis (a type of cell suicide) also decreased.
In another trial, the researchers found that silencing L1TD1 made tumor cells more sensitive to treatment with chemotherapeutic agents. After the procedure, 70% of cultured cells were killed by a dose that would normally have been sufficient to kill only 40%.
For Okamoto, however, the neurosphere assay produced the most interesting result.
“When normal neural stem cells are isolated and grown in the lab, they form structures called neurospheres,” he said. “The same normally happens with medulloblastoma tumor stem cells. In our study, however, L1TD1 silencing reduced neurosphere generation by about 75%.”
Previous research had already shown that the greater the capacity of tumor cells to generate neurospheres, the more aggressive the tumor and the shorter the patient’s survival.
“We also observed that L1TD1 silencing reduced the expression of proteins such as CD133 and nestin that are typical markers of neural stem cells. So there’s a direct correlation between the expression of this gene and the acquisition of stem cell properties,” Okamoto explained. “By inference, we believe this gene is an important factor in tumor proliferation and resistance to chemotherapeutic agents.”
In another study that was part of the research conducted by Carolini Kaid Dávila for her master’s degree, also with support from FAPESP, the group focused on miR-367. Instead of silencing, however, the procedure involved overexpression.
“In the medulloblastoma cell lines we use, expression of miR-367 is relatively weak, and silencing it would probably have little impact. Overexpression, on the other hand, highlights the effect of this microRNA and makes it visible,” Okamoto said.
The group directly injected the tumor cells with synthetic microRNA that mimicked the nucleotide sequence found in miR-367.
“This synthetic microRNA has the same sequence as the original, except for a few minor chemical alterations that make it more stable inside the cell so that it stays there long enough for us to observe the effect,” he explained.
The method was applied to four medulloblastoma cell lines. Proliferation and tissue invasion capacities were found to increase in all lines to a greater or lesser extent.
For Okamoto, however, the most significant result was, again, the increase in neurosphere-generation capacity. “It varied from one line to another, but in some cases it doubled,” he said. “These neurospheres expressed the typical markers of neural stem cells, such as CD133 and nestin.”
In none of the trials performed by the group was the expression of more than one gene altered simultaneously.
“Modifying the expression of a single gene associated with pluripotency was sufficient to change the tumor’s aggressive potential,” Okamoto said. “We therefore believe that interfering in L1TD1 or any other of these genes would be a good strategy to reduce drug resistance and inhibit tumor relapse.”
The article “Embryonic stem cell-related protein L1TD1 is required for cell viability, neurosphere formation, and chemoresistance in medulloblastoma” (DOI: 10.1089/scd.2015.0052) can be read by subscribers to Stem Cells and Development at online.liebertpub.com/doi/10.1089/scd.2015.0052.
The article “miR-367 promotes proliferation and stem-like traits in medulloblastoma cells” (DOI: 10.1111/cas.12733) can be read in Cancer Science at onlinelibrary.wiley.com/doi/10.1111/cas.12733/full.
Republish
The Agency FAPESP licenses news via Creative Commons (CC-BY-NC-ND) so that they can be republished free of charge and in a simple way by other digital or printed vehicles. Agência FAPESP must be credited as the source of the content being republished and the name of the reporter (if any) must be attributed. Using the HMTL button below allows compliance with these rules, detailed in Digital Republishing Policy FAPESP.





