

The EGFR protein, marked in brown, is expressed at differing levels of intensity in penile cancer cases (images: Alice Muglia Thomaz da Silva Amancio)
Research finds a new way to identify high-risk patients who are most likely to benefit from targeted cancer therapy, which uses drugs to block proteins involved in tumor growth.
Research finds a new way to identify high-risk patients who are most likely to benefit from targeted cancer therapy, which uses drugs to block proteins involved in tumor growth.
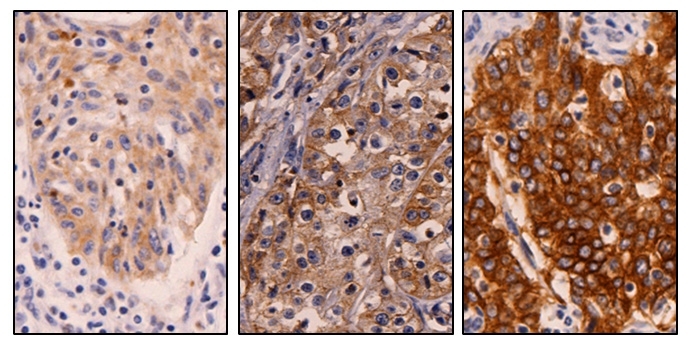
The EGFR protein, marked in brown, is expressed at differing levels of intensity in penile cancer cases (images: Alice Muglia Thomaz da Silva Amancio)
By Karina Toledo
Agência FAPESP – Researchers at the A. C. Camargo Cancer Center in São Paulo, Brazil, have found molecular markers that may help identify patients with penile cancer who are most at risk of dying and likely to benefit from targeted cancer therapy, a form of molecular medicine that uses drugs to block proteins involved in tumor growth.
The research was conducted with support from FAPESP as part of Alice Muglia Thomaz da Silva Amancio’s PhD work, supervised by Fernando Augusto Soares, Director of the A. C. Camargo Cancer Center’s Department of Anatomic Pathology.
Muglia’s research is also within the ambit of the Thematic Project “Cancer of the penis, a real Brazilian problem: from morphology to molecular etiopathogenesis”, coordinated by José Vassallo, Full Professor of Pathology at the University of Campinas (UNICAMP). The findings were presented on March 5 during the A. C. Camargo Cancer Center’s 18th Pathology Meeting.
“Patients with penile cancer are typically poor and cannot afford treatment, which is basically surgical today. Targeted therapy could be an alternative, although it’s costly and requires careful patient selection,” Muglia said.
The disease mainly occurs in developing countries and correlates with poor personal hygiene, phimosis, and infection by pathogens such as human papillomavirus (HPV). Smoking and sex with animals are also considered risk factors.
The incidence of penile cancer in Brazil is estimated at between 2.9 and 6.8 cases per 100,000 inhabitants or approximately 2% of cancer cases in men. According to a 2008 study by the Brazilian Urology Society, the disease typically appears at an earlier age in Brazil than elsewhere and, in most cases, is not diagnosed until it reaches an advanced stage.
The Unified Health System (SUS), Brazil’s national health service, funds approximately one thousand operations per year, mostly in São Paulo State, to amputate all or part of the penis. Conventional treatment with chemotherapy and radiotherapy has not proved effective.
Although distant metastasis is rare, many patients die from treatment complications, especially when removal of the inguinal/pelvic lymph nodes present in the groin is required, Muglia said.
In search of alternatives
“Little is known about the molecular markers of penile cancer. So, for this project we decided to investigate the role played by epidermal growth factor receptor (EGFR), a protein that sends control signals into tumor cells, telling them to grow and divide. EGFR is typically altered in various types of cancer and is therefore a target for therapy,” Muglia said.
Two therapeutic approaches target EGFR. One uses monoclonal antibodies such as trastuzumab that block EGFR activation at the cell membrane. The other uses tyrosine kinase inhibitors (TKIs) such as imatinib that act on the intracellular region of the receptor to prevent growth signals from reaching the nucleus.
The first step to investigate these markers in cases of penile cancer, conducted by Muglia as part of her master’s research, comprised evaluating the expression of EFGR and other proteins in the same family (such as HER2) that are also expressed by cancer cells in a series of 188 tumors removed from patients at the A. C. Camargo Cancer Center.
“These proteins only stimulate growth when they’re found in dimers, or pairs, so it’s important to evaluate them together,” Muglia said.
The results showed that EGFR in particular is strongly expressed in tumor cells, pointing to its therapeutic potential. The cause of this strong expression, however, is unknown.
During her PhD research, Muglia evaluated two factors used as selection criteria for targeted therapy in other neoplasms: the presence of EGFR gene mutations that increase activation of the protein, and gene amplification (growth in the number of copies of the EGFR gene in the genome), which typically leads to increased production of the receptor.
EGFR-activating mutations, which frequently occur in lung cancer, were not found in the penile cancer cases investigated, according to a comment published by the research group in the journal Expert Opinion on Therapeutic Targets. For this analysis, they sequenced 29 tumors in the series. An increase in the number of EGFR gene copies was observed in approximately 25% of the cases.
“The analysis showed that for these patients with EGFR gains, the risk of dying from cancer was four times greater than for the rest. This is as important a variable for assessing prognosis as is the presence of compromised lymph nodes,” Muglia said.
This is the first evidence indicating that EGFR influences carcinogenesis and prognosis, thereby indicating that it could be a candidate target for treating this neoplasm, she added.
As for HER2, the authors observed an increase in copies of not only the gene but also the entire chromosome that contains it, chromosome 17.
This polysomy, which is present in 20% of the analyzed cases, also had a negative impact on survival. Recurrence was about three times higher in patients with the alteration, and they died sooner as a result of the disease (60% of cases with polysomy compared with only 12% of cases without the alteration).
“We hypothesize that the increase in copies of the EGFR gene and chromosome 17 may trigger chromosomal chaos in the cell, resulting in the loss of cell division control and a worse prognosis. The use of targeted therapy would be justified in these cases, as it could help reduce mortality,” Muglia said, adding that only future clinical trials can demonstrate the effectiveness of the treatment.
Republish
The Agency FAPESP licenses news via Creative Commons (CC-BY-NC-ND) so that they can be republished free of charge and in a simple way by other digital or printed vehicles. Agência FAPESP must be credited as the source of the content being republished and the name of the reporter (if any) must be attributed. Using the HMTL button below allows compliance with these rules, detailed in Digital Republishing Policy FAPESP.





